Cycling back pain is a common complaint among all kinds of riders. The lower back can gradually become stiffer and more uncomfortable as long rides go on.
Back pain that intensifies often makes big adventures less enjoyable across road, gravel and mountain biking. Maintaining power, especially on climbs, and staying aerodynamic or nimble on trails is harder when your back is playing up.
In addition, nagging back pain can often persist once you’ve peeled yourself off the bike, sometimes leading to difficulty standing, sitting upright and even sleeping.
This means looking after your back and managing back pain is essential for life on and off the bike
We recommend you seek professional help if your cycling back pain is chronic. But if it’s the occasional niggle, then we have some expert advice that could help.
There’s a lot of overlap between the five most common kinds of pain caused by cycling, so protecting your back can reduce the pain you feel elsewhere.
Below, we explore some of the reasons why you might experience lower-back pain from cycling, and we'll share some suggestions – as recommended by the experts – on how to reduce the symptoms.
- What causes lower back pain from cycling?
- Spinal movement and back pain
- Bike fit and back pain
- Tips to prevent back pain
- Exercises to avoid back pain
What causes lower-back pain from cycling?
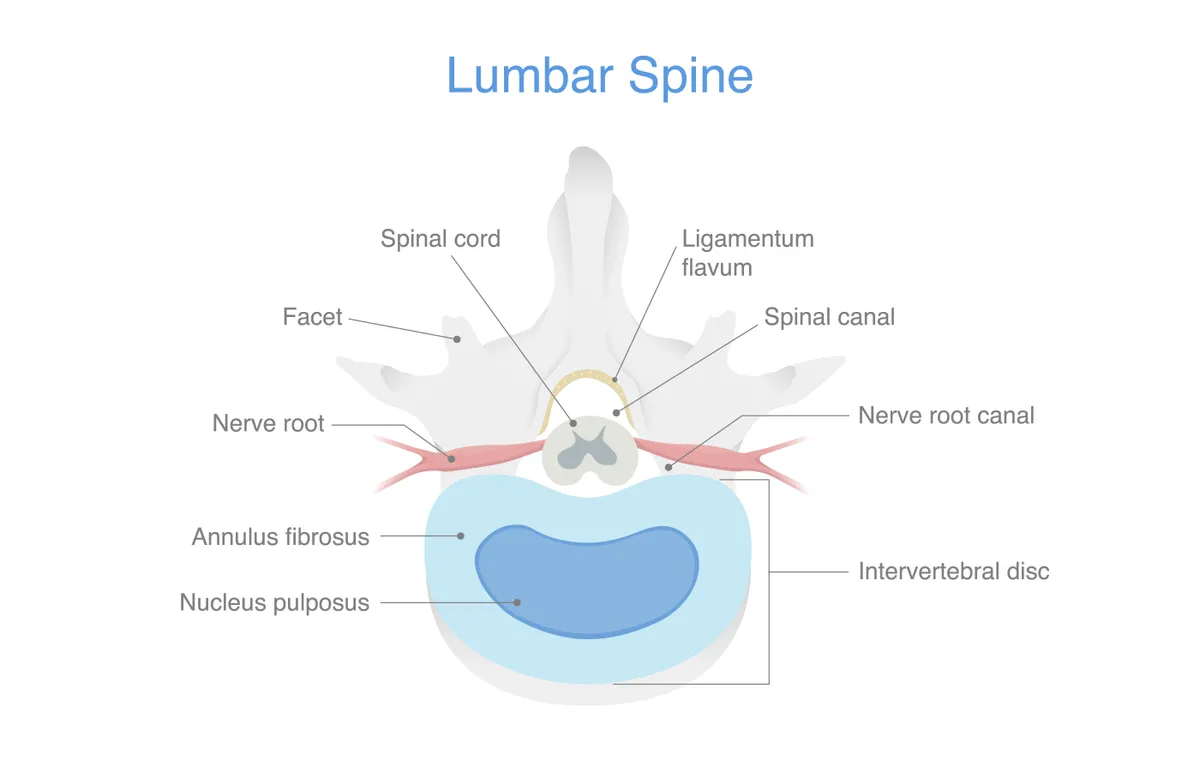
Sport and exercise scientist, Paul Hough, explains how the lower back comprises a mass of muscles, tendons and ligaments. These form a cylinder of musculature around the lumbar spine, which is referred to as the core.
These soft tissues work together to support the spine, maintain posture and initiate movement.
Hough explains that cycling causes “static flexion” of the lower back when we bend forwards to hold the handlebar.
Riding in an aggressive road bike position in the drops exacerbates the bend in the spine, he says.
Hough also states that desk jobs can exacerbate lower-back pain. You should stand up and move every half an hour when working in the office or from your desk at home.
Riders prone to lower-back pain should also be wary of cycling early in the morning, when vertebral column discs are at greater risk of injury, he says.

Physio and bike fitter Phil Burt explains how flexing our lower back while cycling puts the spine into an open joint position, where we are slightly more vulnerable to injury.
But the back is somewhat supported because we are seated in the saddle. However, Phil goes on to say: “This seat can nevertheless transfer a significant amount of vibration into the pelvis and lower back.”
Over time, this leads to pain in your back muscles, which become fatigued and stiff due to the effort of trying to absorb the shock. Then the nerves in your vertebrae take the brunt of the impact.
Meanwhile, Hough explains how poor hip flexor and hamstring flexibility can also contribute to lower-back pain.
Then there's the issue of bike fit – for example, incorrect road bike sizing or road bike position.
If you’re experiencing back pain from mountain biking, our guides to mountain bike sizing and mountain bike setup should help you find the right position and minimise the chance of back pain.

Dr Michael Lanning, a chiropractor who specialises in cycling-related joint and spine injuries, says a cyclist’s back muscles are usually their weakest link.
“Cyclists have huge leg muscles but don’t have the torso strength to support and resist the tremendous forces that the legs can generate,” he explains.
“If the torso is weak that force doesn’t go into the pedals but is dissipated in flexing of the abdomen.
“Look at tired riders – every stroke generates an ‘S’ curve in the back, causing fatigue and muscle spasm.”
No rider will ever develop a sufficiently strong torso through riding alone, he claims.
“Riding with undeveloped abs is something like riding a bike with a cracked frame – all the energy gets dissipated in flexion, and doesn’t get you down the road.”
Joy Potts, an osteopath and sports injury specialist, believes some riders’ back pain traces back to crashes.
“I see so many riders who spend hours and hundreds of pounds sorting out their bikes after a crash, but don’t think twice about their bodies," she says.
“Without you realising, it can cause the pelvis to become twisted and make your legs different lengths – issues that create muscle imbalances and put huge pressure on your lumbar spine as you twist your abdomen for power.
“Always, always get a professional once-over after any crash. Leave it too late and it can result in months of pain,” she advises.
Weakness in other areas can force the lower-back muscles to overwork, leading to fatigue and back pain.
The obliques stabilise the torso when you climb out of the saddle. But if they are too feeble to do so, your climbing power will diminish and your back muscles take up the load.
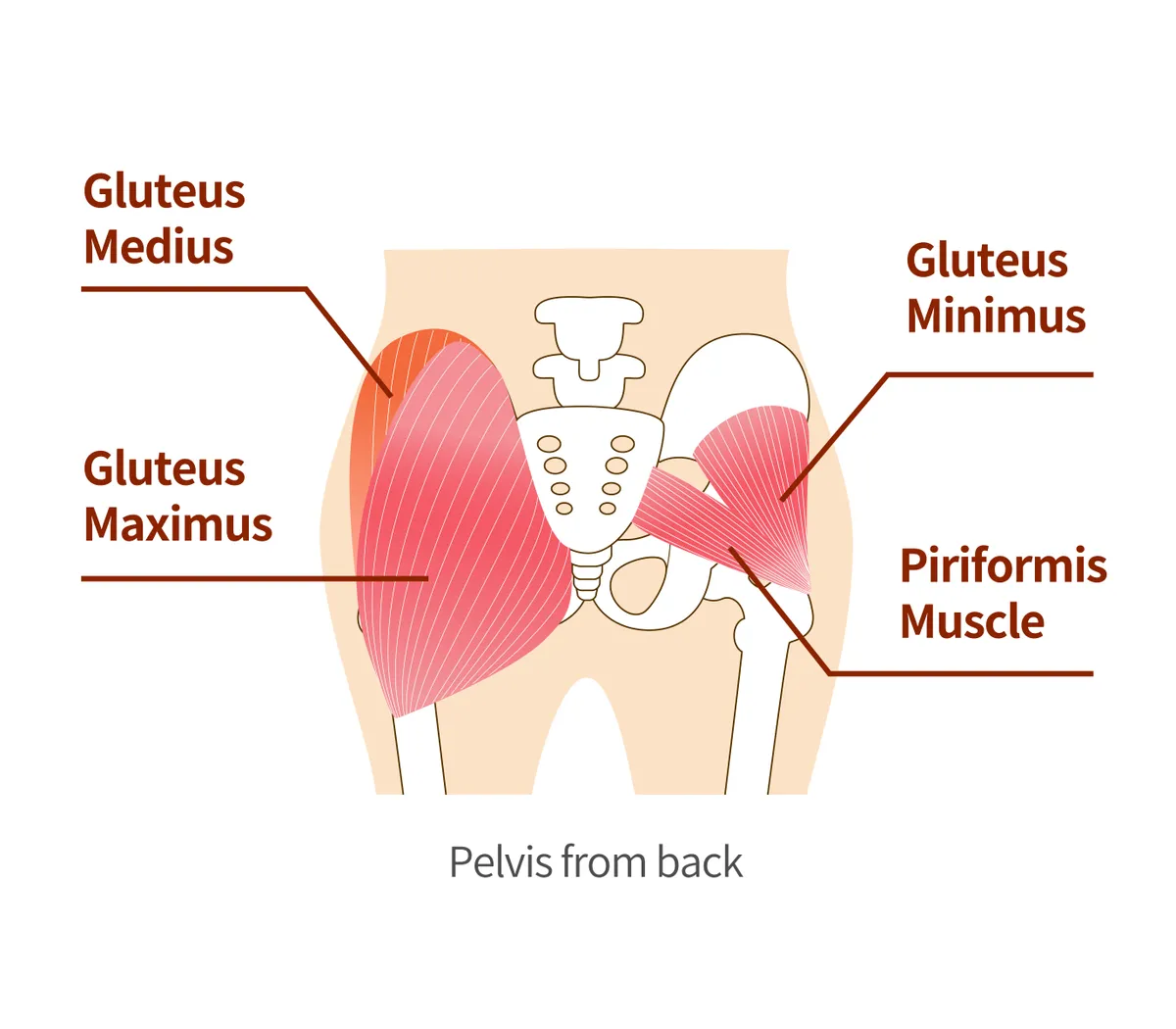
The glute medius is a muscle that can cause lower-back pain from cycling. We rarely use it day to day, but cycling requires more of this muscle found on the outside of the buttocks.
“It literally holds your pelvis in place so you get an efficient transfer of power in the lumbar region,” says Paul Massey, a British Olympic Association physio.
A weak glute medius tires quickly and leaves more of the work supporting your pedal-stroke to the back muscles.

Poor pelvic position can also lead to back pain from cycling, Potts adds. “Tight quads will tilt the pelvis forward, while tight hamstrings will tilt it back.
“In both cases, your lower back will overarch and start to take the strain when it should be your much bigger muscles in the core,” says the osteopath.
Low cycling cadence is another potential cause. So be careful if you’re training to become a hill climbing star.
Pushing bigger gears or overdoing your hill sets can overly fatigue the glutes and hamstrings, again leading to pain.
What about upper-back pain?

Upper-back pain and neck pain are most often caused and exacerbated by riding position and technique, explains elite cycling coach Andy Wadsworth.
Riding in drop handlebars for long periods will not only increase the load on the arms and shoulders, it will also hyperextend the neck.
“Prolonged hyperextension leads to ‘trigger points’, small rubbery knots that form in muscle and adjacent fascia muscle sheaths, which send pain signals to the brain and contribute to a pain-spasm-pain cycle,” says Wadsworth.
If the virtual top-tube length (top tube plus stem length) is too long for the rider, or if aero bars are used, hyperextension is a near certainty, he claims.
“It’s especially common in the early season when riders are increasing both their mileage and the time they spend in the saddle.”

The other common causes of upper-back pain are simple problems in the muscles, says GP Andy Ward.
“This can be due to poor posture, prolonged sitting at a computer, weakness of the muscles, using a backpack, repetitive strain or minor injury.
“A more serious cause might be suggested by pain after a heavy crash, a history of osteoporosis, age at onset less than 20 or over 50 years, previous cancer, fever, weight loss, night pain, prolonged symptoms or numbness, pins and needles or weakness in the arms and legs,” he continues.
Dr Ward warns against carrying heavy loads in a backpack on the bike and suggests using a rack and pannier bags instead.
But if you do wear a cycling backpack, Dr Ward says you should pack it carefully.
“The amount of weight carried is more important than bag design, and a stable, symmetrical load is associated with fewer muscle problems,” he advises.
Spinal movement and cycling back pain

Paul Hough says cyclists with a lot of flexion in the lumbar spine are at higher risk of experiencing lower-back pain.
More spinal movement can leave the core muscles underdeveloped, tight and unbalanced, he adds.
However, bike fitter Bianca Broadbent claims your spinal area can also be too rigid for cycling.
“Cycling, unlike many other sports, does require us to hold a relatively static position, so good muscular endurance is helpful,” she says.
She adds you don’t want your body to rotate as you pedal, but some truncal stiffness helps comfort and performance.
Bike fit and back pain

Bike fit plays a big role in ensuring you are comfortable on the bike and safe from injury.
Potts says getting your bike saddle height right is crucial for reducing the chances of back pain when cycling.
“If your saddle is too high, you’ll rock side to side, causing the muscles between your pelvis and lower back to spasm,” she says.
“Put your heel on the pedal at the six o’clock position and sit on the saddle – your leg should be almost straight and you shouldn’t have to rock your hips to reach down.”
Andy Wadsworth says if you suffer from neck pain you should also inspect the setup and fit of your bicycle.
You might find you have to raise the handlebar or change to a bar with a shallower drop or greater rise, if you’re using a flat mountain bike handlebar. You could also reduce the virtual top-tube length with a shorter bike stem.
“Moving the saddle forward should also reduce virtual top-tube length, but be careful as a poor saddle position can lead to knee issues, which are just as hard to sort when they set in,” Wadsworth cautions.

Bike fitter Phil Cavell says your position on the bike depends on a variety of factors.
“The optimal distance and drop of the bar from the saddle depends on your body’s capabilities, specifically hamstring length, lower-back flexibility and functional core,” he explains.
As a result, the less core strength and flexibility you have, the closer and higher the bar needs to be.
Read our ultimate guide to bike geometry and handling to find out more.
Matt Bottrill, former British national time-trial champion and coach, argues a professional bike fit can ward off back pain while cycling.
He says improved glute activation and back comfort come with saddle setback and saddle angle, while lower back and shoulder comfort come with stem length and bar height.
“All of these things will improve your efficiency on the bike and reduce the accompanying risk of injury,” says Bottrill.
Tips to prevent lower-back pain from cycling
From gradually increasing your training load to fitting wider tyres, here’s how you can protect your back from pain.
Build up slowly
Cranking up training too fast can cause cycling back pain.
To avoid early-season over-use injuries, Andy Wadsworth suggests initially riding at a high cadence and low resistance, and only increase training mileage by 10 per cent a week, gradually building to goal mileage.
Strengthen your core

Bianca Broadbent explains: “A strong core will optimise your ability to produce power because you will have a more solid base.
“Core musculature is not just limited to the abdominals,” she says. “It includes the spinal extensors in your back, leg muscles, such as your glutes, and the deep postural muscles that work at lower thresholds for longer periods of time to help maintain a stable position. All of these muscles contribute to core strength.”
To hone your glute medius, Olympic physio Paul Massey recommends performing three sets of 10 side leg raises twice a week.
To do a side leg raise, lie in a straight line on your side. Slowly lift your top leg directly vertical as far as you can.
Keep the opposite hip pressed to the floor or mat. Consider placing your top hand on your glute medius (the side of your backside) to make sure you’re feeling it working.
Gently lower the top leg to the starting position.
This exercise also works your transverse abdominals, a major muscle of the functional core.
Flexibility

When you pedal, your legs are the pistons that drive you along, but your bottom, lower back and abdominal musculature are also working hard, especially as you climb.
The position you hold on the bike puts extra strain on your core. You’ll be rounding your spine to some degree, regardless of how upright your riding position is, and putting strain through your back as a result. Flexibility is as important as core strength.
Potts says stretching can stop tight muscles pulling your pelvis out of shape.
“The key message is you need to strengthen your core away from the bike before your back takes the strain. Focus on stretching to maintain pelvic position even when you’re dog-tired," she says.
We have an in-depth article on stretches to improve your flexibility and cycling performance. It’s also worth doing foam roller exercises to roll out tight muscles.
Wider tyres

Physio Phil Burt believes higher-volume road bike tyres have reduced his clients' back pain from cycling.
“During my time at British Cycling, as well as at Team Sky, if a rider had a lower-back injury we would automatically widen the tyres they were using,” he says.
“In road cycling, the aim has always been to improve comfort by trying to absorb some of the forces the road throws up to the rider vertically: the bumps and shudders.
“The increased air cushion (and therefore volume) a wider tyre provides is hard to beat in terms of achieving this goal.”
Medical help
Some riders swear by a spinal treatment called Advanced Biostructural Correction.
Among them is BikeRadar’s senior mountain bike technical editor Alex Evans, who believes chiropractors can help with cycling back pain.
Hough warns that sudden, acute pain or ‘pins and needles’ can be symptoms of a herniated disc or sciatica. You should speak to a physiotherapist or osteopath before trying any exercises to resolve these issues.
Ward highlights cost-effective ways to deal with back pain. “Acute pain can be treated with paracetamol and anti-inflammatories, but always read the label to check if they are safe for you. Ice packs can also help reduce discomfort.
“If symptoms are severe or unresponsive, seek medical advice," he says. “And, if any of the risk factors associated with serious problems are present, this should happen sooner rather than later.”
Exercises to avoid cycling back pain

“You need to incorporate core stability, flexibility and conditioning drills into your training to make your time in the saddle more comfortable,” says Paula Coates, author of Back Pain: Exercise Yourself to Health.
Paula suggests carrying out a combination of the following exercises on a regular basis to help avoid back pain from cycling.
“Mix and match the following exercises and stretches in a simple 20-minute workout twice a week, and in just a month you will see noticeable improvements,” she says.
Walking lunges

- Targets: Quads, core and hip flexors
- 3x 15-20 reps
1. Step forward into a lunge position, bending the front knee and ankle to 90 degrees, which will help you keep your knee behind your toes.
Keep your weight on your back leg and clench your buttocks.
2. Dig your front heel into the floor and step the other leg forward into the lunge position.
Keep your steps wider than your pelvis because this will increase your base of support and stability.
The cat stretch
- Targets: Spine and core
- Unlimited – repeat little and often
1. Kneel on all fours, with your knees a hip-width distance apart and your hands a shoulder-width apart.
This can also be done sitting on your bike.

2. Imagining your pelvis is a bucket filled with water – tilt your pelvis forwards and backwards for one to two minutes as if you were tipping water out of the front and back of the bucket.

The Bug
- Targets: Core
- 3x 10 breaths
1. Lie on your back with your arms reaching towards the ceiling and your hips and knees bent to 90 degrees.
If this feels too difficult, you can support your legs on a gym ball or on the arm of your sofa.

2. Making sure your spine is flattened gently against the floor and your pelvic floor is lifted, hold this position as you gently breathe in and out.
Repeat three times for 10 breaths, resting between each set.
You should feel this in the tummy not the back; if you have back pain, wait until you’re stronger or reduce the time you hold the position.
Variation 1: Arm float – as you breathe out, slowly raise your left arm over your head, then breathe in and return your arm to the start position.
Repeat with your right arm and alternate each arm for 30 seconds, increasing to one minute as you become stronger.

Variation 2: Leg floats – as you breathe out, slowly lower your left foot towards the floor, but only as far as you can while keeping a neutral spine.
Breathe in and return the hip to the start position.
Repeat with your right foot.
Alternate legs for 30 seconds, increasing to one minute as you become stronger.

Crucifix stretch
- Targets: Lumbar spine and hips, buttocks, back muscles and hamstrings
- 2x 10-15 reps
1. Lie on your back with your arms stretched out at right angles to your sides and both your legs straight, as if you’re on a crucifix.
Keep your arms in contact with the floor at all times.

2. Lift your right leg 2 inches off the floor and swing your leg across your left leg, as far as it will comfortably go. Your right toes should now be towards your left hand.
3. Return your right leg to the starting position and repeat with the left leg. Do two sets of 10 to 15 repetitions.
If your flexibility is poor or you’ve had a flare-up of lower-back pain, bend your knees, keeping your feet on the floor, and roll your knees from side to side.
Dynamic hamstring stretches
Targets: Hamstrings, piriformis, tensor fasciae latae and calf
10-20 reps in each position after every ride
1. Standing with your feet together, take three small steps (heel to toe) so you stop with one foot in front of the other.

2. Lean forward and slide your hands down your leg to your ankle.
The forward movement should come from your lower back and your hips.

3. Take three more small steps so your opposite foot is in front – again reach your hands down to your ankle.
Repeat 10-20 times.
4. The next stretch starts in the same way – take three small steps but turn the toes of your front foot out with the outer side of your heel level with the big toe on the back foot.
Repeat 10-20 times.
5. The final stretch starts in the same way with three small steps, but this time turn the front foot in, keeping the inside of your heel level with the big toe on the back foot.
Thoracic extension stretch
Targets: Spine and chest
Daily 15-20 minutes
1. Use an exercise ball, or roll up a small towel to a diameter of 10-15cm and secure with elastic bands.
2. Lie on the ball or, if using a towel, a bed with the towel lengthways down your spine, from the base of your neck to the middle of your back.

3. Raise your arms to either side of your head and let them hang or rest on the bed.
If this is too much of a stretch, support or rest your arms on pillows to reduce the pull across your chest.





