If you're suffering from knee pain from cycling, we're here to help you identify where the discomfort's coming from, what's causing it and how to stop it.
Our guide covers the areas of the knee where pain might be felt when riding a bike, and the specific conditions that can lead to knee pain when cycling.
We also take a close look at the inner workings of the knee and explain how cycling overuse injuries can lead to problems that stem from three broad categories.
Each of these will have contributory factors from three problem domains:
- Changes in training intensity (cycling-specific)
- Changes in equipment (bike-specific)
- Our intrinsic anatomical and biomechanical make-up (cyclist-specific)
The key is to identify which of these is the cause of your cycling knee pain and make a change.
Read on to boost your knee knowledge and banish needling pain.
Remember the golden rule for cycling knee pain
While we can give you some basic strategies for getting out of trouble when plagued by knee pain, the old adage rings true: stay out of trouble in the first place.
- Many problems with the knee can be avoided by not making sudden increases in your training regime or drastic changes in bike setup.
- Look after your legs and they’ll look after you: stretch all the big muscle groups after each ride and treat them to the odd massage.
- Don’t neglect core muscle strength – smaller core muscles can relieve much bigger limb muscles of surprisingly large loads.
The scope of this article is limited to some of the more common overuse injuries, so if you’ve sustained an acute injury or experience sudden pain, or if your symptoms don’t improve with this very general advice, please seek appropriate qualified medical help.
The four main areas of knee pain for cyclists
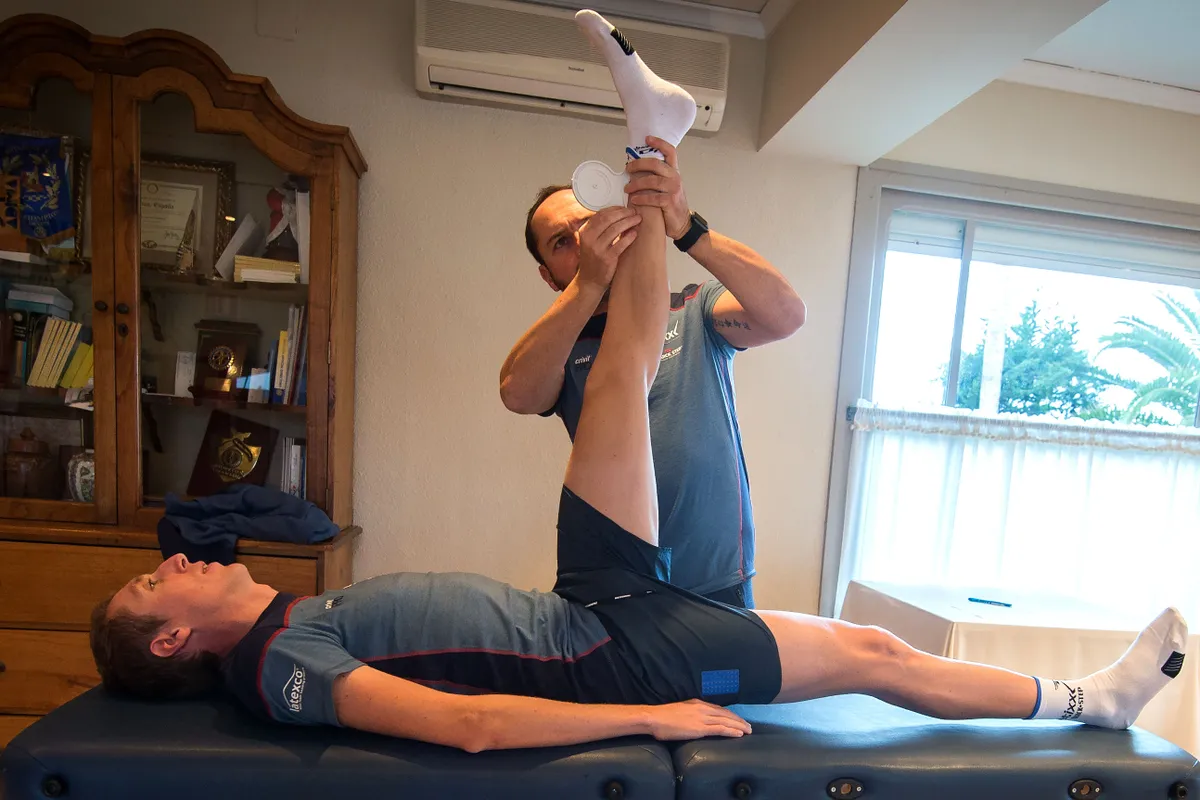
There are four areas of knee pain: anterior, posterior, medial/lateral and iliotibial band syndrome. Let's look at each of those in turn.
Area 1: Anterior knee pain
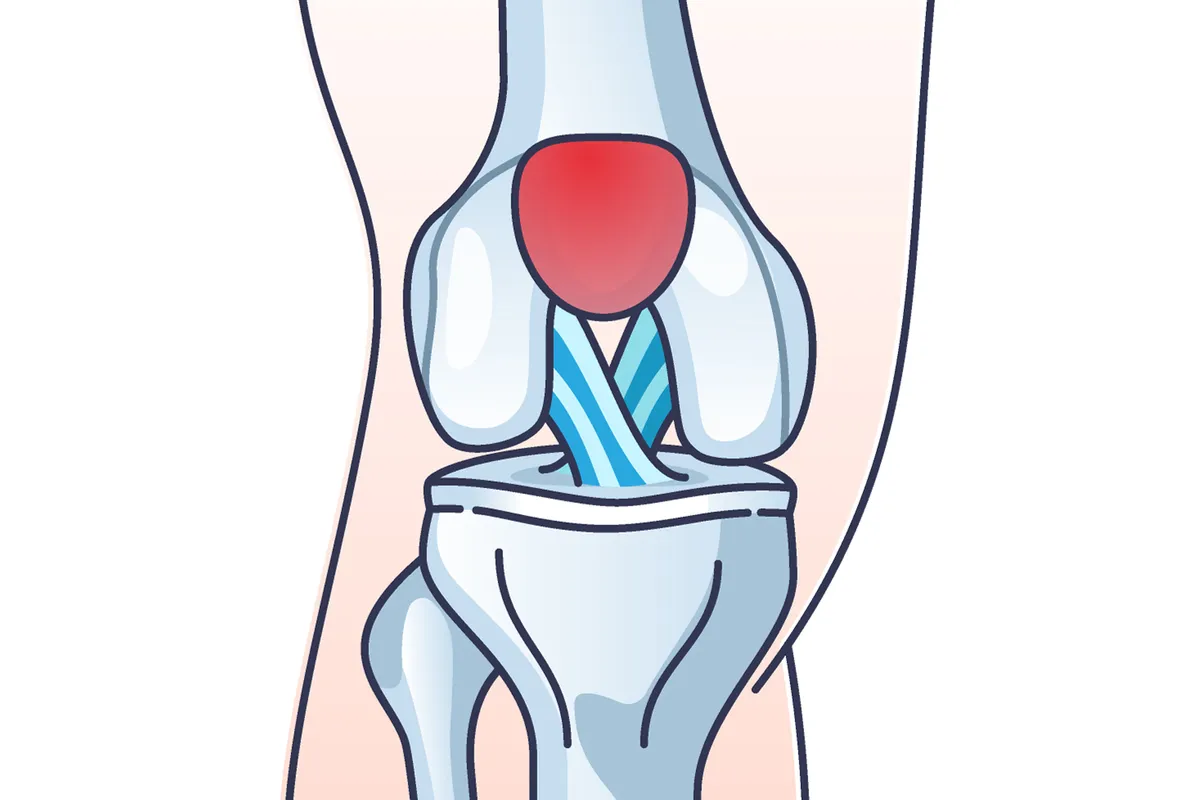
Pain at the front of the knee – on and around the knee cap (patella) – is the most common presentation of cycling overuse injuries and one of the most common women-specific cycling injuries.
it is sometimes referred to as spring knee, which typically occurs when cyclists ramp up their mileage after training less in winter.
The large quadricep muscles attach to the shin bone via the patella, so the forces of pedalling are transmitted across the patello-femoral joint whenever we bend our knees, essentially squashing it back against the thigh bone.
Although more common in explosive sports, the part of the tendon attaching the patella to the bony prominence below the kneecap can become inflamed (patellar tendonitis). If this area is persistently sore to the touch it’s definitely worth seeking medical help. It should respond to ice, anti-inflammatories and physiotherapy, with or without strapping.
However, if you’re reading this and you have anterior knee pain from cycling, chances are you’ve got what’s known as a 'patellar compression syndrome'.
The scourge of cyclists and runners alike, it can completely floor you, causing pain when off the bike and ride-stopping agony when on it.

During the push phase of pedalling, we seldom complete the last 35 degrees of knee extension – a movement which is largely under the control of the vastus medialis oblique (VMO) muscle.
This means that over a long period of time, and often in spite of outward appearances, the muscles down the outside of the thigh become much stronger and tighter than these less-used medial muscles.
The patella is pulled subtly off-kilter and forces through the patello-femoral joint increase, causing diffuse pain anywhere around the kneecap. The soft tissues around the lateral aspect of the patella slowly shorten over time, and make strengthening exercises of the VMO muscle alone largely ineffectual.
Four ways you can treat anterior knee pain when cycling

The key to treating such a condition is to loosen off the lateral structures before attempting to redress the balance and concentrating on building medial muscle bulk.
There are various methods for doing this, all of which aim to reduce the forces through the patello-femoral joint:
- Try to keep your leg out straight, if you’re troubled with anterior knee pain of this type, whenever you have the choice.
- Be aware of bike-specific problems. Make sure your saddle is set to the right height. Pushing too big a gear or using excessively long cranks can also be a problem.
- Building up the vastus medialis oblique muscle can also help. Start by regularly stretching and massaging the lateral side for a week or so. Then begin work on building up the vastus medialis oblique muscle with exercises such as wall/ball squats or lunges. This will help balance out the stabilising forces on the patella, and in a couple of weeks you’ll feel a difference.
- There’s not much point in taping up the patella because the forces generated when cycling are too great and the taping just won’t hold. Particularly resistant cases can be tackled by a sports physio, who can work specifically on mobilising the tight lateral tissues around the patella.
It’s also worth pointing out that cycling isn’t the only time we bend our knees and stress the patello-femoral joint.
Crouching down to pick something up and tackling stairs are more obvious activities, but sitting at a desk with feet underneath the chair (or in a cinema seat) for prolonged periods will produce the same effect.
Area 2: Posterior knee pain
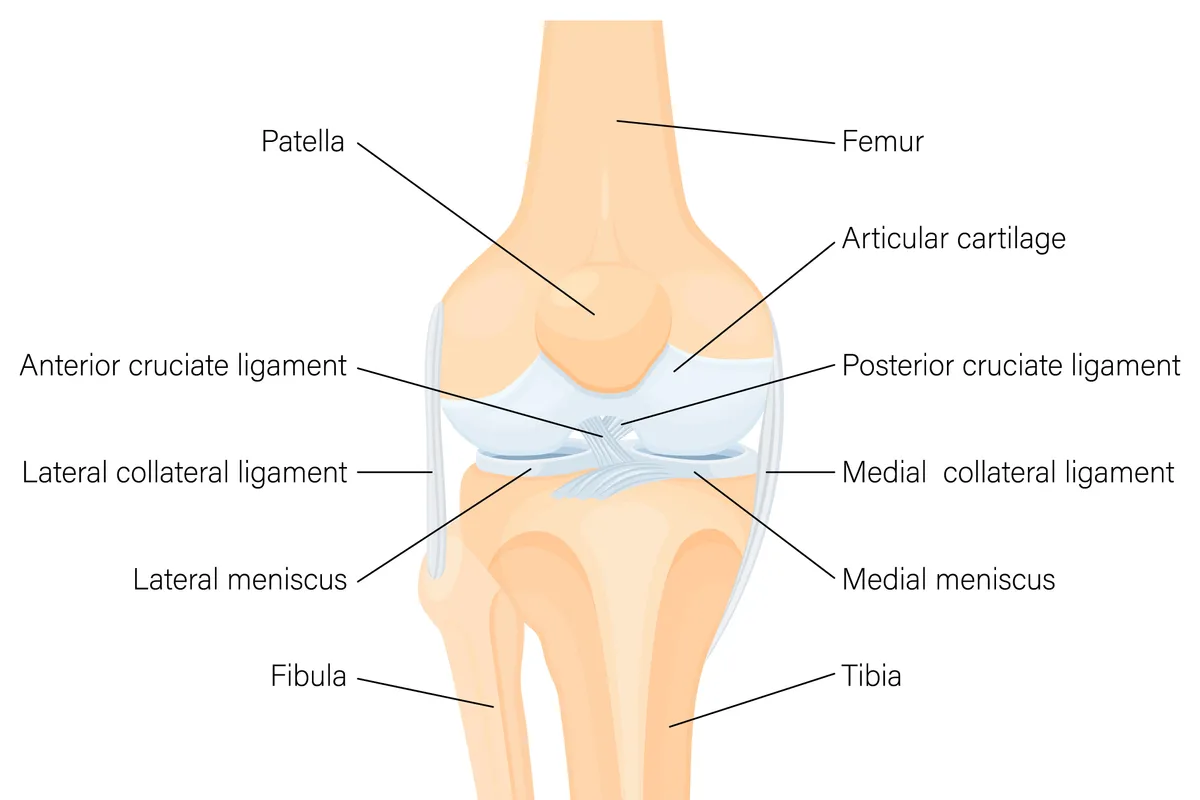
Pain behind the knee is far less common, and much more straightforward. It’s almost always due to over-extending the knee.
- Bike-specific problems to look for: a saddle that’s too high or too far back, although these are just as likely to cause pain further up the hamstrings.
Persistent pain behind the knee should be looked at medically to exclude a Baker’s Cyst.
Named after the person who originally described them and nothing to do with making bread, they’re a harmless bulging of synovial fluid into the space behind the knee. Your doctor can discuss treatment options with you.
Area 3: Medial and lateral knee pain
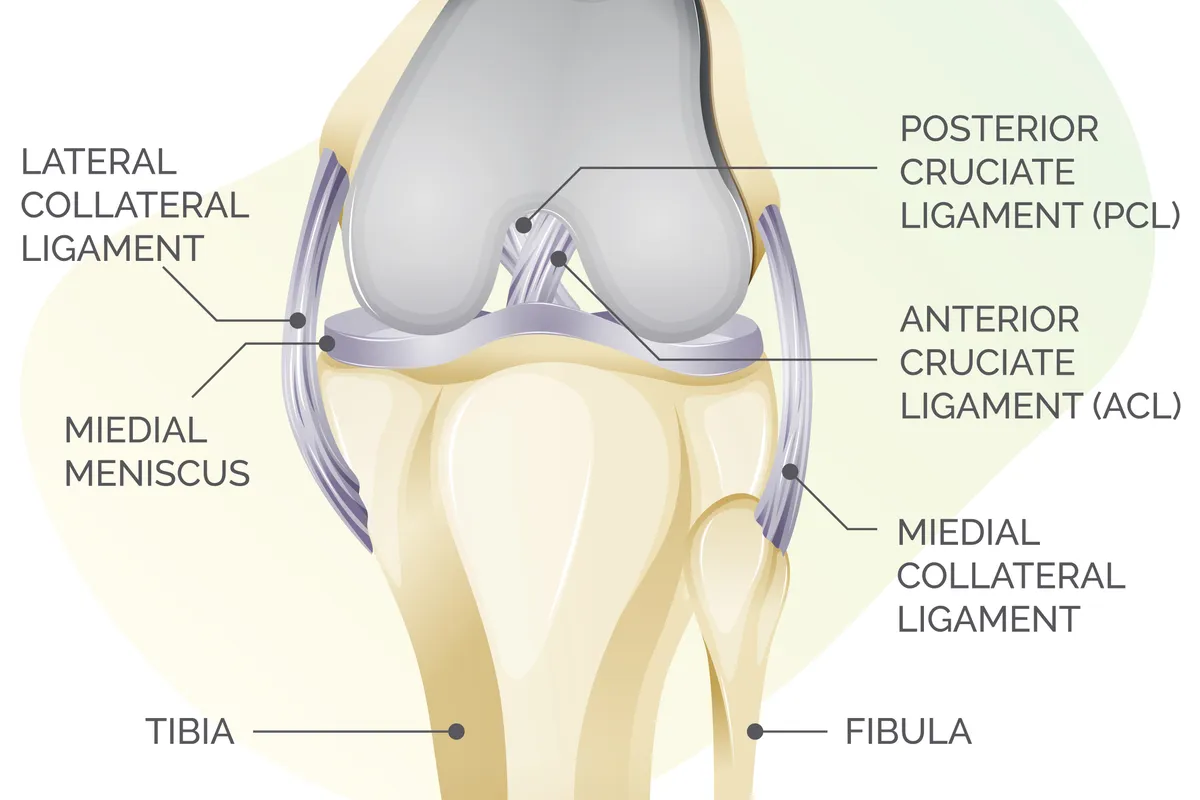
Pain at the sides of the knees is fairly common and the culprits here are almost always the feet, or more specifically, incorrectly fitted pedal cleats.
To this end, such pain is often noticed during or after the first ride with cleats, or with a new pair of shoes or replacement cleats.
The structures causing the pain are most often the collateral ligaments, which sit on the outsides of the knee joints, stopping them from bending the wrong way.
- Bike-specific problems are usually to blame here: badly placed cleats will either affect the Q angle (how far apart your feet are positioned) or cause excessive rotation of the knee joint, stressing one or other of the collaterals. The cleat position and knee pain diagram (below) describes the usual culprits and what to do with them.
Two ways to avoid and treat medial and lateral knee pain when cycling
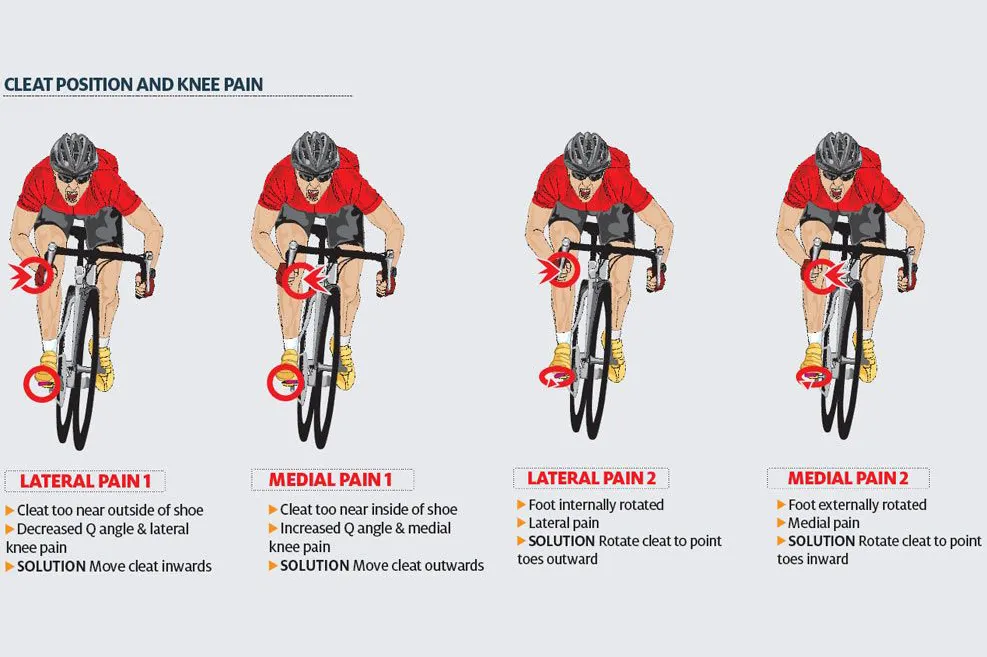
- Check cleats for excessive wear regularly. Always make sure you draw round cleats with a felt tip pen to mark your position before replacing them. Experiment with different cleat types until you find one with the right amount of float for you (too much or too little can both cause problems).
- Get off on the right foot. If you’re new to cleats, one tip for getting a good starting position is to sit on the edge of a table with hips, knees and ankles relaxed at 90 degrees. Look down: whatever angle your feet naturally dangle at should be replicated by the cleats.
Area 4: Iliotibial band syndrome

Another painful condition that’s very closely related to patellar compression syndrome is called 'iliotibial band syndrome'.
The iliotibial band is a thick fibrous strap of tissue that runs all the way down the lateral thigh, from the pelvis to just below the knee. It’s a structure that has a habit of tightening up over time and pulling the patella off centre if your vastus medialis oblique muscles aren’t strong enough to counteract.
Because of where it sits, as the knee is repeatedly bent and straightened, it moves back and forth over the knobbly end of the thigh bone just above the knee, cushioned by a fluid-filled bursa. It’s at this point that inflammation can occur, which is then irritated each time the knee is bent.
Most commonly seen in runners, it’s an unpleasant condition thought to be exacerbated by weakness of the gluteus medius muscle – another essential core muscle that gets neglected by cycling – and also by wearing cleats that point the toes too far inwards.
How to manage iliotibial band syndrome

In the acute phase of the injury, the mainstay of its treatment is the same as any for an inflammatory condition: rest, ice and regular anti-inflammatory medications such as Ibuprofen, if tolerated.
Rehabilitation after this is very similar to that described above for patellar compression syndrome, but with a focus on building up the gluteus medius muscle instead of (or as well as) the vastus medialis oblique.
Near-religious stretching, especially of the iliotibial band, should precede strengthening exercises. A return to normal activities should be phased in gradually, being guided by (a lack of) pain. Incredibly resistant cases can be operated on, but it’s rarely required if the above regime is followed.
Gluteus medius strengthening exercises for cyclists
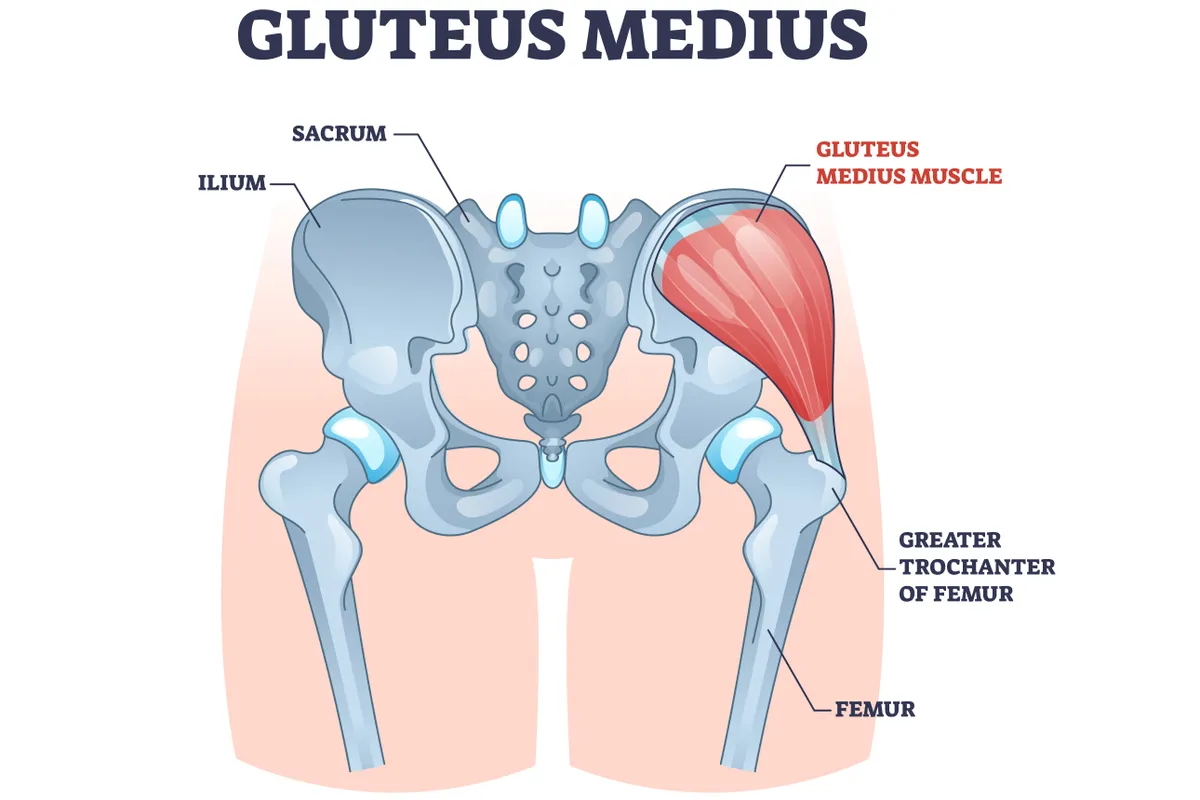
The following exercises are all designed to strengthen and loosen the gluteus medius muscle – an important core abductor of the hip, often neglected by cycling.
It’s a smallish muscle which, when contracting, can be felt as a lump at the top of the 'scoops' of your buttocks – it’s a good idea to place a hand on this area when doing the exercises, to make sure you’re exercising it.
1. Side-lying leg lifts
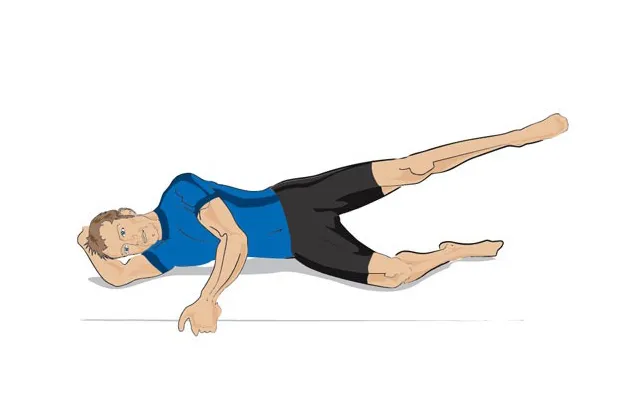
Lie on one side on a mat with your legs straight. Slowly lift the top leg until you feel your gluteus medius is working.
Then lower the leg back perpendicular to the mat and repeat. Do 2-3 sets of 10-12 reps.
To increase resistance as you progress, add ankle weights or loop an exercise band around your shins.
2. Side-lying quad stretch
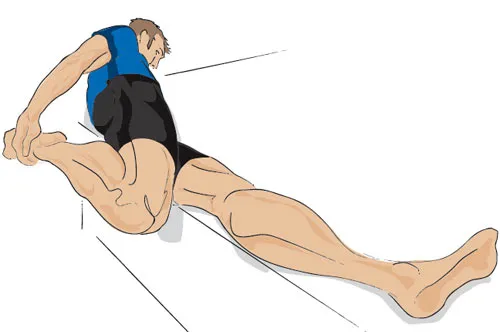
Lie on your good side, in a straight line along the edge of a bed so you're looking across the bed.
Hold on to the end of the bed with your lower arm for support.
Reach behind you with your upper arm and pull your foot to your bottom, as if you were doing a regular quads stretch. Keeping your foot against your bottom, gently increase the quads stretch by pulling your leg backwards. You'll feel it along the front of your thigh – let yourself relax into this stretch.
Still holding this stretch, and making sure you don't tilt your hips backwards, now very gently push your knee down towards the floor.
At a certain point you should feel quite a sharp stretch down near the knee – perfect for lengthening those tight soft tissues around the lateral aspect of the patella. It's important to keep your whole body in line and perpendicular to the bed during the stretch.
3. Upper iliotibial band stretch
Standing upright, cross your bad leg behind your good one, making sure you keep it locked straight.
Then, without bending forwards, gently lean sideways from the waist over to the good side.
You can support yourself against a wall by leaning away from it. You should feel this stretch over the outside of the hip and upper thigh.
4. Massage
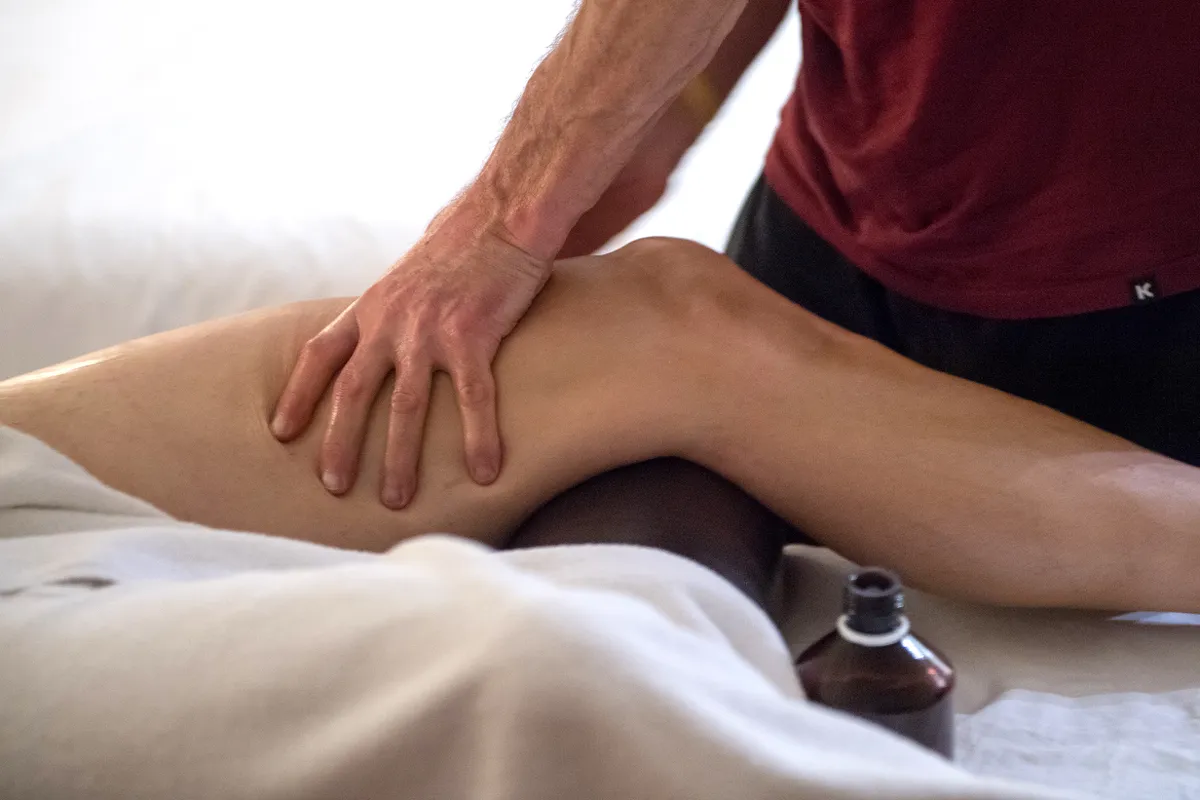
You can do this yourself, after a ride or a hot bath. With the leg locked out straight, rub with firm pressure all along the outside of the thigh. This is most easily achieved by using the palm of your hand to rub a squash ball in a circular motion over the muscles.
Alternatively, use a little oil and the flats of your fingers or thumb. If you're really lucky, you'll have a willing helper to do it for you.
5. Trigger points

This doesn't work for everyone, but applying deep, sustained pressure (for up to 30 seconds) with a thumb or foam roller over particularly tight or painful areas along the lateral thigh can sometimes work wonders. Sit down, lock your leg out straight to relax all the quads and find problem areas by massaging.
Pressing hard can cause your eyes to water if you're feeling particularly tender, but persist with it and you'll often feel tight spots twitching in submission and relaxing under the pressure.
An indirect and effective way of pinpointing these trigger points is to lie on your side and gently lower the weight of your leg on to a tennis ball. Be warned though, it's not for the faint-hearted.
